While people are discovering the many ways chiropractic care enhances well-being, doctors of chiropractic are commonly associated with a sore back. It doesn’t matter that modern chiropractic was born in 1895 when D.D. Palmer restored a janitor’s hearing with a spinal adjustment.
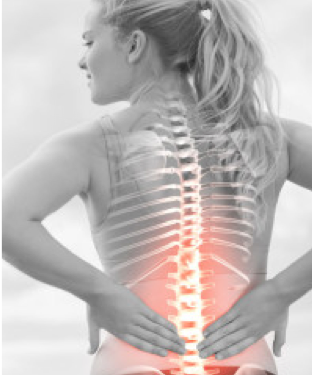
Back pain, and low back pain in particular, soon stole the stage with its effectiveness in relieving the often-crippling symptoms. With good reason, it seems. In the past year alone, according to the 2018 Gallup-Palmer College of Chiropractic study, “Managing Neck and Back Pain in America,” 25 percent of Americans sought professional health-care in treating their neck and back pain. And nearly two-thirds of us will experience severe enough pain to seek care in our lifetimes.
That is why the Foundation for Chiropractic Progress has designated low back pain as its focus in December. It is an issue escalated by the opioid epidemic as people want options to the prescription painkillers that often lead to addiction, abuse and overdose. Multidisciplinary health care is emerging, with medical organizations such as the American College of Physicians encouraging people to try chiropractic care before taking opioids or considering surgery. Americans have strong opinions of their own as well, as seen in the recent Gallup-Palmer College of Chiropractic study.
One in four – 28 percent – prefer drug- and surgery-free treatment, though eight out of 10 – 79 percent – want options. And one in five of those with significant back and neck pain take prescription painkillers. Medical physicians and doctors of chiropractic are the top choices – 62 and 53 percent, respectively – the latter chosen because they provided the most effective treatment, the study said.
Americans’ trust is well placed. According to a 2018 study of active-duty military personnel, participants experienced fewer back problems when treated with chiropractic and medical care. As Christine Goetz, who led the research, has noted, “This study provided the strongest evidence to date that chiropractic is safe, that it’s effective and that it can be integrated into a multidisciplinary health care setting.”
Americans also try to deal with pain on their own, applying heat or ice, practicing yoga, getting a massage or using over-the-counter pain relievers, which can also be risky when overused.
And there are effective actions you can take to complement your chiropractic care:
• Make lifestyle changes now that prevent back and neck pain. Good posture is a good place to start. Avoid becoming sedentary—breaking away from the desk for stretches and regular exercise. Drink plenty of water, and while you are at it, watch what you eat as well. Your doctor of chiropractic can suggest additional measures you can take specific to your situation.
• Seek treatment at the first sign of back pain. Watch for stiffness or decreased range of motion in the neck, a knot in the back muscle, loss of bladder or bowel control, loss of balance or coordination, muscle weakness or numbness and tingling in your extremities. While they may not seem related to the back, they often originate from the spine … your doctor of chiropractic’s area of expertise!
• Keep your healthcare professionals informed on what you are experiencing and what other treatments or prescriptions you are receiving. We are at the crossroads in addressing an issue dating back to the beginning of time. And recent studies – along with dialogues scheduled own the road – indicate that we are on the same page in pursuing relief.